Optimization Tip: How To Use ABR Click Polarity Wisely…
Brainstem auditory evoked potentials can be a pain. Sometimes downright frustrating. Their saving grace is that anesthesia is really going to have to go out of their way to mess up the responses. We might see some absolute latency increase in our waves, but waveform morphology, amplitude size, and interpeak latencies should not be affected.
There are 2 main reasons why they can be so bothersome.
First, a lot of the cases I’ve done using BAER have a big honking tumor compressing on the nerve. Sure, I’ve used them in other cases like microvascular decompression of cranial nerves (CN 5, 7 and 9 are the ones I’ve done personally), Arnold Chiari malformation and brainstem tumors, but CPA tumors have been a large percentage. The larger the tumor, the bigger the problem.
Second, the amplitudes are so small. And the smaller the waveform you’re trying to collect, the more susceptible to the noise they are. Wave V is your largest short-latency response in ABR (assuming no pathology, these all should all come in less than 10ms) and a well-formed wave will have an amplitude around 0.5uV. Wave I and III are usually around or less than 0.25uV. Compare that to something like an SSEP that comes in around a couple uV, and you can see why the recommended traces needed to collect a response is about double that of somatosensory evoked potentials.
But there are some tricks you can use to try to obtain better brainstem auditory evoked potentials. Choosing from a couple of different stimulation polarities may help you in a pinch. But before I go into when to use which, let’s make go over exactly what they are and how they affect our auditory system differently.
In the operating room, we deliver a broadband click through foam inserts placed in the ear canal. The purpose of using a broadband instead of frequency specific tone-burst is it is more efficient and creates that classic wave I, III and V appearance that we are all used to seeing.
But those “classic” waves will be affected in appearance by the way you set up your recording electrodes, as well as the way you stimulate CN 8.
When we think about using sound as a stimulator, it might be easiest to imagine a drum. But not beating the drum with a stick, but the effects of atmospheric pressure on it. A negative atmospheric pressure is going to pull it out, and a positive atmospheric pressure is going to push it in. The way the drum effects the tympanic membrane of the ear (pushes or pulls it) is going to affect the basilar membrane in the same manner, but at slightly different times.
BAER Stimulator Polarities
The stimulators we use in the OR are capable of delivering either rarefaction or condensation clicks separately or in an alternating pattern. So let’s give some definition to each.
First is Rarefaction. This one is a crowd favorite when I talked to some of the audiologists who transitioned to intraoperative neuromonitoring. It is the most common polarity used in diagnostic ABR. So even though it isn’t the recommended polarity in the operating room, this is still the default starting polarity for some of them.
Rarefaction causes a negative pressure and moves the elastic diaphragm away from the tympanic membrane. Think of it as pulling it away. The effect on the waveforms is seen greatest on the wave I, where it increases the amplitude and decreases the latency and helps to separate wave IV off of wave V. In some cases, this might be beneficial in order to better visualize a true wave V.
Condensation, also commonly called compression, causes a positive pressure and moves the elastic diaphragm towards the tympanic membrane. Think of this as pushing it towards it. The effects of condensation are greatest seen on wave V, causing it to have a larger amplitude. In some cases, where wave V amplitude is borderline unreliable due to amplitude size, you may want to check the waves using this polarity. It should be noted that this is the least commonly used stimulus polarity used.
It should be noted that if you go back and read some of the literature in the 70’s and 80’s when they were making these comparisons of click polarities, it wasn’t an all-or-none outcome. A large percentage of their subjects (around 60%) presented with a shorter latency and larger amplitude of wave I using rarefaction, around 15% had shorter latencies and larger amplitudes with condensation and the rest it didn’t matter. There is still some understanding that needs to happen with the way the basilar membrane reacts to this stimulation, effects in different intensities and rates, effects of certain hearing loss and adaptation to responses in central processes.
Finally, the alternating click is a delivery of a rarefaction click followed by a condensation click. It decreases stimulation artifact and eliminates cochlear microphonic. This is important because the cochlear microphonics can bleed over wave I, especially when high intensities are used, making it unreliable. Alternating click polarity is the most commonly used polarity in the operating room, although it should be noted a possibility of phase cancellation and distortion of the response, particularly in newborn and in adults with high-frequency hearing loss, is possible.
Knowing what your primary objective in the operating room is for collection brainstem auditory evoked responses, you now have a reason to start with alternating click polarity and make changes accordingly.
But this is all considerations made for baseline assessment.
If you switch from rarefaction to condensation, you will see an inversion in your cochlear microphonics, but there will also be changes in your wave I latency, alterations in wave I-V interpeak latencies and wave V/I ratio because of the effects of switching stimulation.
In patients with high frequency hearing loss and hearing loss due to neuropathologies, not only was the wave I and V latencies affected, but wave V amplitude responses were dependent on stimulus polarity. All this happens even though rarefaction and condensation stimulation are spectrally and perceptively identical just because of the initial influence on the earphone diaphragms. The reasoning is unknown.
But that’s important information to know. I would recommend not changing polarities after you set your baselines, seeing as you can cause a change in your waveform recordings that could mimic a significant change and cause you to incorrectly alarm the surgeon.
Working backwards
I think the best way to present this information is by showing how you would use it in the operating room. We know what to start with when to try a different polarity and what to expect when a change is made. That’s the steps that the in-the-room clinician goes through if troubleshooting is needed.
But what about the remote physician? They get a ding on their chat box asking for their input on baselines, and possibly a request on how to better optimize responses. They might not have seen the troubleshooting that was taking place, or know exactly how the recording and stimulating parameters are setups. Their initial view is typically the traces up to that point. It would be in their best interest to be able to look at a waveform and say to themselves…
“oh, I see XYZ, which means they are using ____ as their stimulation polarity. The traces look like (blah, blah). They might be able to better optimize wave (I, III or V) if they switched to _____ polarity.”
So let’s try looking at it from that point of view, going through that thought process. What would you recommend in the following situations:

Joe Hartman
Subscribe to our Awesome Newsletter.
Keep Learning
Here are some related guides and posts that you might enjoy next.
Intraoperative Neuromonitoring – The Complete Guide…
This is your guide to understanding the field of intraoperative neuromonitoring, from the perspective of a patient, surgeon, or potential surgical neurophysiologist. It will cover exactly what intraoperative neuromonitoring is, who can do it, how it's done, and more....
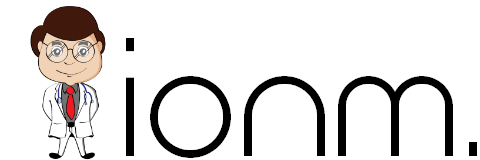
How To Run Hypoglossal Nerve Stimulation For Obstructive Sleep Disorder
Hypoglossal Nerve Stimulation: A Novel Technique for IONM This isn't our first time helping surgeons map out nerves. We are starting to see some traction in hypoglossal nerve stimulation for obstructive sleep apnea. Obstructive sleep apnea is one of the most prevalent...
The CNIM Is JUST A Luxury Item: Part 2
Blasphemy! I wasn't intending to do a follow-up post, but I've been catching some heat lately. Comments. Text. Even phone calls. You know something just hit the fan if people actually use their phone to call you. I touched a nerve when I called the CNIM a luxury item....
How To Avoid An Unimpressive IONM Resume…
What Does Your IONM Resume Say About You? Let's break down the neuromonitoring field a little bit here (it will help your IONM resume not suck)... If you had to guess what percent of the cases your company monitors are spine cases, where would you place your bets? If...
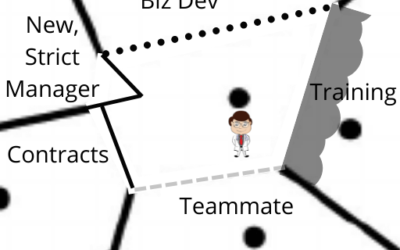
Changing My Mind on TIVA For Carotid Endarterectomy?
Beliefs Are Identities In hindsight, it was obvious. It almost always is. But this one seems like a real head smacker. I don't need any modern equipment; 30 minutes and a playground and my 2 boys will make a bulletproof case for handwashing. Their fingernails will...
The CNIM Is JUST A Luxury Item (But Not How You Think)
What Is Your CNIM Worth? Imagine this: You go to school for 4+ years -- purposely putting yourself into debt -- only to realize the job you want only overlaps this expensive education on the margin. So far, you're in pretty good company with most students coming out...
Help Spread The Word. Social Media Works!




0 Comments